Secure, speedy, and reliable : Up to 70% Off!!!
Diabetes and Diabetes Symptoms: Early Warning Signs You Should Never Ignore
Learn about diabetes and diabetes symptoms, including early warning signs, causes, risk factors, and prevention tips to protect your health.
3/1/20269 min read
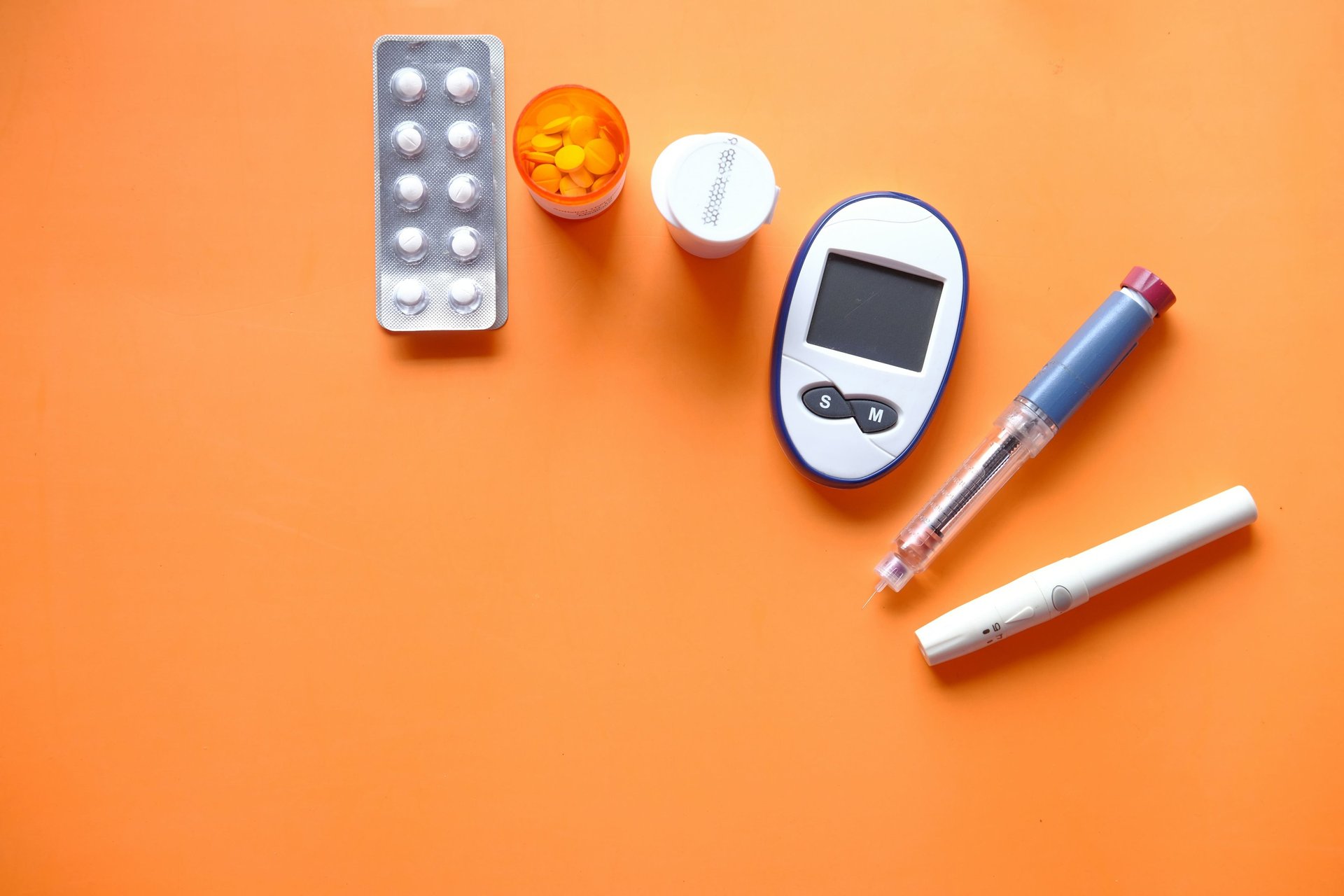
Introduction
Diabetes is one of the most common chronic health conditions worldwide, affecting millions of people across all age groups. Despite its prevalence, many individuals remain unaware of the early diabetes symptoms until the condition progresses to a more serious stage. Recognizing the warning signs early can make a significant difference in preventing long-term complications and improving overall health outcomes.
Diabetes occurs when the body either does not produce enough insulin or cannot effectively use the insulin it produces. Insulin is a vital hormone that regulates blood sugar levels and allows glucose to enter cells for energy. When this process is disrupted, blood sugar levels rise, leading to a range of symptoms and potential health risks.
Understanding diabetes and diabetes symptoms is essential for early detection, proper management, and prevention. In this article, we will explore the different types of diabetes, the early warning signs you should never ignore, the causes and risk factors, possible complications, and practical strategies for prevention and management.
1️⃣ What Is Diabetes? Understanding the Condition
Diabetes is a chronic medical condition that affects how your body processes blood sugar (glucose). Glucose is the primary source of energy for your body’s cells. It comes from the foods you eat and travels through your bloodstream to provide fuel for muscles, tissues, and organs — especially the brain.
To understand diabetes, it’s important to understand the role of insulin.
The Role of Insulin in Blood Sugar Control
Insulin is a hormone produced by the pancreas, a small organ located behind the stomach. Its job is to act like a key, allowing glucose in the bloodstream to enter the body’s cells where it can be used for energy.
When you eat:
Your blood sugar levels rise.
The pancreas releases insulin.
Insulin helps glucose enter cells.
Blood sugar levels return to normal.
In people with diabetes, this system does not work properly. Either the body does not produce enough insulin, or it cannot use insulin effectively. As a result, glucose builds up in the bloodstream instead of being used for energy. Over time, high blood sugar levels can damage organs, blood vessels, and nerves.
The Main Types of Diabetes
Understanding the different types of diabetes helps clarify why symptoms and treatment approaches vary.
Type 1 Diabetes
Type 1 diabetes is an autoimmune condition. The immune system mistakenly attacks and destroys insulin-producing cells in the pancreas. As a result, the body produces little or no insulin.
Often diagnosed in children and young adults
Requires lifelong insulin therapy
Symptoms can develop quickly
Type 2 Diabetes
Type 2 diabetes is the most common form. It occurs when the body becomes resistant to insulin or does not produce enough of it.
Often linked to lifestyle factors
Develops gradually
More common in adults, but increasingly seen in younger people
Can sometimes be managed with diet, exercise, and medication
Gestational Diabetes
Gestational diabetes develops during pregnancy in some women. It usually disappears after childbirth but increases the risk of developing Type 2 diabetes later in life.
Why Early Understanding Matters
Many people live with diabetes for years without knowing it, especially in the case of Type 2 diabetes. During this silent phase, high blood sugar may already be causing internal damage.
By understanding what diabetes is and how it affects the body, individuals are better equipped to recognize early diabetes symptoms and seek medical advice promptly.
Early diagnosis and proper management can:
Prevent serious complications
Improve quality of life
Reduce long-term health risks
2️⃣ Early Diabetes Symptoms You Should Never Ignore
One of the most dangerous aspects of diabetes is that early symptoms can be mild, gradual, or easily mistaken for everyday fatigue or stress. Many people, especially those with Type 2 diabetes, may live with elevated blood sugar for years before receiving a diagnosis. Recognizing early diabetes symptoms is critical to preventing serious long-term complications.
Here are the most common warning signs you should never ignore:
1. Frequent Urination (Polyuria)
If you find yourself urinating more often than usual — especially waking up multiple times at night — this could be an early sign of diabetes.
When blood sugar levels are too high, the kidneys work harder to filter and remove excess glucose from the bloodstream. This process pulls more water into the urine, increasing both frequency and volume.
Persistent frequent urination is one of the body’s first signals that blood sugar is out of balance.
2. Excessive Thirst (Polydipsia)
Because frequent urination causes fluid loss, your body becomes dehydrated. This leads to increased thirst, even if you are drinking more fluids than usual.
Many people describe this symptom as:
Constant dry mouth
Feeling thirsty all the time
Drinking large amounts of water without feeling satisfied
When excessive thirst and frequent urination occur together, it strongly suggests abnormal blood sugar levels.
3. Extreme Fatigue
Glucose is your body’s primary energy source. When insulin is not working properly, glucose cannot enter your cells efficiently. As a result, your body lacks usable energy — even though there is plenty of sugar in your bloodstream.
This leads to:
Persistent tiredness
Low energy despite adequate sleep
Difficulty concentrating
Unlike normal tiredness, diabetes-related fatigue does not improve easily with rest.
4. Unexplained Weight Loss
Sudden weight loss without changes in diet or exercise can be a warning sign, particularly in Type 1 diabetes.
When the body cannot use glucose for energy, it begins breaking down fat and muscle instead. This leads to unintended weight loss, sometimes occurring rapidly.
If you lose weight without trying, especially along with increased hunger or thirst, medical evaluation is important.
5. Blurred Vision
High blood sugar can cause fluid shifts in the lenses of your eyes. This affects your ability to focus properly, leading to blurry or fluctuating vision.
While this symptom may come and go, persistent blurred vision should never be ignored. Over time, uncontrolled diabetes can lead to serious eye complications.
6. Slow Healing Wounds and Frequent Infections
Elevated blood sugar impairs circulation and weakens the immune system. As a result:
Cuts and bruises take longer to heal
Skin infections may occur more frequently
Gum infections can become more common
Women may experience recurrent yeast infections
If minor wounds seem to linger for weeks, it may signal underlying blood sugar imbalance.
Why Early Detection Matters
These early diabetes symptoms may appear gradually and seem harmless at first. However, untreated high blood sugar can silently damage the heart, kidneys, nerves, and blood vessels.
The good news is that early diagnosis allows for effective management through lifestyle changes, medication, and regular monitoring.
If you experience multiple symptoms listed above, especially in combination, consulting a healthcare provider for blood sugar testing is essential.
3️⃣ Risk Factors and Causes of Diabetes
Understanding the risk factors and causes of diabetes is essential for prevention, early detection, and effective management. While some risk factors cannot be changed, many are directly linked to lifestyle habits — meaning there are powerful steps you can take to reduce your risk.
The causes of diabetes vary depending on the type, but all forms involve problems with insulin production, insulin function, or both.
Causes of Type 1 Diabetes
Type 1 diabetes is considered an autoimmune condition. This means the immune system mistakenly attacks and destroys the insulin-producing beta cells in the pancreas.
Although the exact trigger is not fully understood, researchers believe it may involve:
Genetic susceptibility
Viral infections that trigger immune response
Environmental factors
Type 1 diabetes is not caused by diet or lifestyle habits. It often develops in childhood or adolescence, though it can occur at any age.
Because the body produces little to no insulin, lifelong insulin therapy is required.
Causes of Type 2 Diabetes
Type 2 diabetes is far more common and develops differently. It occurs when:
The body becomes resistant to insulin (insulin resistance), and
The pancreas cannot produce enough insulin to compensate.
Unlike Type 1 diabetes, Type 2 is strongly influenced by lifestyle and metabolic health.
Over time, excess blood sugar builds up, leading to the symptoms and complications associated with diabetes.
Major Risk Factors for Diabetes
Several factors significantly increase the likelihood of developing Type 2 diabetes:
1. Overweight and Obesity
Excess body fat — especially around the abdomen — increases insulin resistance. Abdominal fat is particularly linked to metabolic dysfunction.
2. Physical Inactivity
Regular movement helps the body use insulin more effectively. A sedentary lifestyle reduces insulin sensitivity and increases blood sugar levels.
3. Unhealthy Diet
Diets high in:
Processed foods
Sugary beverages
Refined carbohydrates
Trans fats
can contribute to weight gain, insulin resistance, and metabolic imbalance.
4. Family History
If a parent or sibling has diabetes, your risk increases. Genetics play a significant role in how your body handles blood sugar.
5. Age
Risk increases after age 45, although Type 2 diabetes is now being diagnosed more frequently in younger adults and even teenagers due to lifestyle changes.
6. High Blood Pressure and Cholesterol
Cardiovascular risk factors often overlap with diabetes risk. Metabolic syndrome — a cluster of conditions including high blood pressure, high blood sugar, and abnormal cholesterol — significantly raises diabetes risk.
7. History of Gestational Diabetes
Women who developed gestational diabetes during pregnancy are more likely to develop Type 2 diabetes later in life.
The Good News: Many Risks Are Preventable
While you cannot change your genetics or age, you can influence many major risk factors. Maintaining a healthy weight, staying physically active, and following a balanced diet can dramatically reduce your chances of developing Type 2 diabetes.
Early awareness of risk factors allows individuals to take preventive action before blood sugar levels reach dangerous levels.
4️⃣ Complications of Untreated Diabetes
Diabetes is not just about elevated blood sugar — if left unmanaged, it can silently damage nearly every organ system in the body. Understanding the potential complications underscores why early detection and proper management are critical.
1. Heart Disease and Stroke
High blood sugar levels damage blood vessels and nerves that control the heart. This increases the risk of:
Heart attacks
Stroke
High blood pressure
Atherosclerosis (hardening of the arteries)
People with diabetes are two to four times more likely to develop cardiovascular disease than those without diabetes.
2. Kidney Damage (Diabetic Nephropathy)
The kidneys filter waste from the blood, but prolonged high blood sugar can damage tiny blood vessels in the kidneys. Over time, this may lead to:
Chronic kidney disease
Kidney failure requiring dialysis
Protein leakage in urine
Regular monitoring of kidney function is essential for people with diabetes.
3. Nerve Damage (Diabetic Neuropathy)
Elevated blood sugar can injure nerves throughout the body. Symptoms may include:
Tingling, numbness, or pain in the hands and feet
Digestive issues such as constipation or diarrhea
Sexual dysfunction in both men and women
Nerve damage increases the risk of injuries and infections, especially in the lower extremities.
4. Eye Damage (Diabetic Retinopathy)
Diabetes can damage the small blood vessels in the retina, leading to:
Blurred or fluctuating vision
Partial vision loss
Complete blindness if untreated
Regular eye exams are essential for early detection and treatment.
5. Increased Infection Risk
High blood sugar weakens the immune system, making it easier for infections to take hold. Common issues include:
Skin infections
Urinary tract infections
Gum disease
Slow-healing wounds
Unchecked infections can escalate quickly, especially in combination with nerve damage.
6. Foot Problems
Nerve damage and poor circulation in the feet can lead to:
Ulcers
Severe infections
In extreme cases, amputation
Daily foot care and regular medical checkups are critical for preventing serious complications.
Why Proper Management Is Critical
While complications are serious, they are largely preventable with:
Consistent blood sugar control
Regular medical checkups
Healthy lifestyle choices
Proper medication or insulin use
Early detection of diabetes and prompt management significantly reduces the risk of long-term health problems.
5️⃣ Preventing and Managing Diabetes Effectively
While diabetes can be serious, it is also highly manageable — and in many cases, preventable. Lifestyle choices, regular monitoring, and timely medical interventions can dramatically reduce risks and improve quality of life.
1. Maintain a Healthy Diet
Nutrition is a cornerstone of diabetes management and prevention. Key strategies include:
Eating whole grains, vegetables, fruits, and lean proteins
Limiting sugary beverages and processed foods
Watching portion sizes to avoid overeating
Balancing carbohydrates with protein and healthy fats to stabilize blood sugar
A registered dietitian can provide a personalized meal plan for both prevention and management.
2. Regular Physical Activity
Exercise improves insulin sensitivity, helping the body use blood sugar more efficiently. Recommended activity includes:
150 minutes per week of moderate-intensity aerobic activity (e.g., brisk walking, swimming, cycling)
Strength training at least 2–3 times per week
Incorporating movement into daily routines, like taking stairs or short walking breaks
Even small, consistent activity can make a big difference.
3. Monitor Blood Sugar Levels
Regular monitoring helps track your glucose and adjust your routine as needed:
Home blood sugar testing with a glucometer
Continuous glucose monitoring (CGM) for those with insulin dependence
Keeping a log of readings, diet, and exercise for better patterns recognition
Monitoring allows early detection of spikes or drops before they become serious.
4. Medication and Insulin Therapy
Some people may require medication or insulin therapy to control blood sugar:
Oral medications (like metformin) improve insulin sensitivity or reduce glucose production
Insulin therapy supplements the body’s natural insulin
Following prescribed dosages and schedules is critical for effectiveness
Medical guidance ensures the right treatment plan for your specific needs.
5. Lifestyle Adjustments
Beyond diet and exercise, other habits support diabetes prevention and management:
Maintain a healthy weight
Quit smoking and limit alcohol intake
Manage stress, as stress hormones can affect blood sugar
Get adequate sleep, ideally 7–9 hours per night
Regular check-ups with your healthcare provider
Adopting these habits can prevent the onset of Type 2 diabetes and reduce complications in those already diagnosed.
Conclusion for the Section
Diabetes doesn’t have to control your life. With informed choices, consistent monitoring, and professional support, it’s possible to manage blood sugar effectively, prevent complications, and maintain a healthy, active life.
Conclusion
Diabetes is a complex but manageable condition. By understanding what diabetes is, recognizing the early symptoms, and being aware of risk factors, you can take proactive steps to protect your health. Untreated diabetes can lead to serious complications, but with timely intervention, lifestyle changes, and proper medical care, it is possible to live a full and healthy life.
Early detection and consistent management are the keys. Monitoring blood sugar, maintaining a healthy diet, staying active, and following medical guidance can prevent complications and improve overall well-being. Remember — knowing the signs and acting early can make all the difference.
Taking control of your health today can lead to a stronger, healthier tomorrow. Don’t ignore the warning signs — your body will thank you.
References for “Diabetes and Diabetes Symptoms”
American Diabetes Association. “Standards of Care in Diabetes—2026.” Diabetes Care, 49(Suppl. 1): S1–S290, 2026.
Source for types of diabetes, symptoms, and management.
Centers for Disease Control and Prevention (CDC). “Diabetes Symptoms.” 2025.
Source for early warning signs and complications.
Mayo Clinic. “Diabetes.” Updated 2025.
Source for causes, risk factors, and prevention strategies.
World Health Organization (WHO). “Diabetes Fact Sheet.” 2025.
Global prevalence, types, and health impacts.
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). “Diabetes Overview.” 2025.
Source for complications, lifestyle recommendations, and medical interventions.
Harvard T.H. Chan School of Public Health. “Type 2 Diabetes Prevention.”
Source for diet, exercise, and lifestyle preventive measures.
Contact
Questions? Reach out anytime, we're here to help.
© 2025. All rights reserved.


